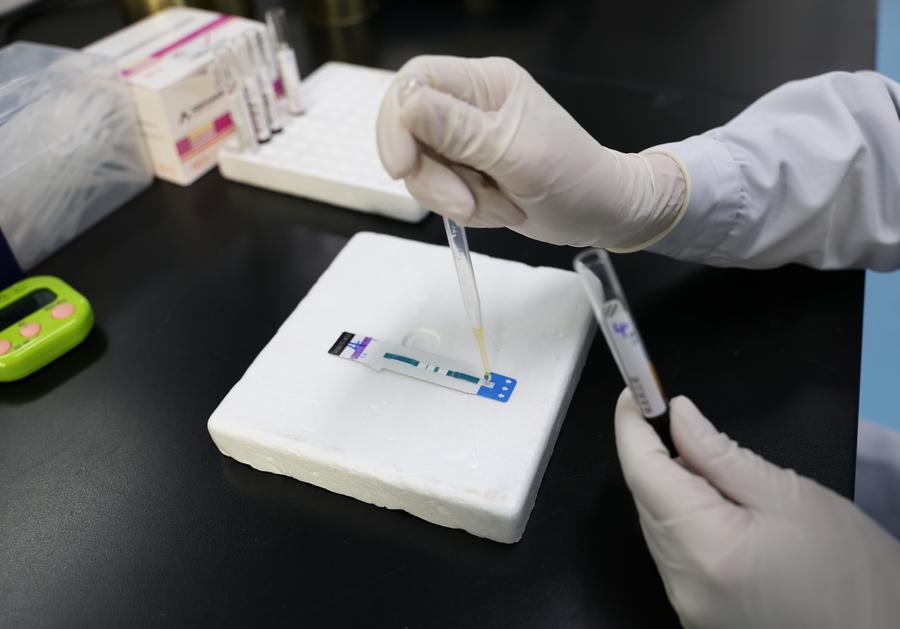
Africa-Press – Eritrea. A doctor tests a sample for HIV/AIDS infection at the Fourth People’s Hospital of Nanning, in Nanning, South China’s Guangxi Zhuang Autonomous Region, Nov. 21, 2024. (Xinhua/Jin Haoyuan)
A Norwegian man has entered long-term HIV remission following a stem cell transplant from his brother, in a rare medical outcome that is drawing global scientific attention.
According to France 24, the 63-year-old man, now dubbed the “Oslo patient” underwent the transplant as part of treatment for blood cancer.
The Oslo patient, who had been living with HIV since 2006, was diagnosed with a fatal blood cancer called myelodysplastic syndrome in 2017.
His doctors searched for a donor who would help treat both. When they couldn’t find one, they chose the man’s elder brother.
The procedure was not initially intended to cure HIV, but subsequent developments have shown no detectable active virus in his body.
Doctors say the transplant involved stem cells from a donor carrying a rare genetic mutation known as CCR5-delta-32. This mutation prevents HIV from entering and infecting immune cells, effectively making the new immune system resistant to the virus.
“We had no idea… That was amazing,” doctor Anders Eivind Myhre of the Oslo University Hospital told AFP.
The researchers found no trace of the virus in samples of the man’s blood, gut and bone marrow.
“For all practical purposes, we are quite certain that he is cured,” Myhre said.
Following the procedure, the patient continued on antiretroviral therapy for a period before eventually stopping treatment under close medical supervision. Years later, there has been no sign of the virus rebounding, indicating sustained remission.
The case adds to a small number of similar instances worldwide where patients have achieved long-term HIV remission after undergoing stem cell transplants. These procedures typically replace a patient’s immune system with one that is naturally resistant to HIV.
However, medical experts caution that such cases do not yet amount to a widely applicable cure. Stem cell transplants are complex, high-risk procedures usually reserved for patients with life-threatening conditions such as cancer.
They can lead to serious complications, including immune rejection and infections.
As a result, this approach is not considered a practical solution for the millions of people living with HIV globally, most of whom rely on lifelong antiretroviral therapy to manage the virus.
Nonetheless, researchers say each successful case provides valuable insights into how HIV can be controlled or potentially eliminated from the body.
Scientists are now studying these rare outcomes to better understand the mechanisms behind them and to explore safer, more accessible treatment options.
Efforts are ongoing to develop alternatives, including gene-editing techniques that aim to replicate the protective effects of the CCR5 mutation without the need for a transplant.
Globally, HIV remains a major public health challenge, with millions of people living with the virus. While current treatments allow patients to lead long and healthy lives, they do not eradicate the virus completely.